01-23-2017, 03:58 AM
(This post was last modified: 01-23-2017, 04:08 AM by vsheline.)
RE: How Long Before Centrals Subside
(01-18-2017, 10:56 AM)hartikka Wrote: I videotaped my night as well last night and noted that I had 3 times where I started up with a few centrals (they were also less in length at about 13sec each). Each time the centrals started I had moved to the supine. Each time I moved to my side the centrals stopped. Hmm?
Hi hartikka,
It is interesting that the CAs were occurring when you were sleeping on your back and went away when you turned onto your side. I don't know whether it is more common for CAs to occur when sleeping on our back.
Is the way you know you were having Central Apneas because (1) you looked at them in SleepyHead and (2) they are marked as CA in SleepyHead and (3) the Flow waveform shows the period of apnea ended with the Flow waveform starting gradually to increase (small inhalation and exhalation, followed by larger inhalation and exhalation, followed by still larger), with the envelope smoothly building back up to normal?
A gradual re-starting of breathing after an apnea is a clear indication that the apnea was central in type.
Even if the machine marks an apnea as central but the apnea ends (breathing restarts) very suddenly with immediately larger-than-average breaths (instead of breaths gradually returning to normal) this is an indication that there was an obstructive component to the apnea, that although at the start of the apnea the airway was open, before the apnea had been ended (by the sudden hard breathing and disturbance/arousal to a more shallow stage of sleep) the airway had collapsed and had become obstructed.
The Advisory Member group provides advice and suggestions to Apnea Board administrators and staff on matters concerning Apnea Board operation and administrative policies. Membership in the Advisory Member group should not be understood as in any way implying medical expertise or qualification for advising Sleep Apnea patients concerning their treatment.
RE: How Long Before Centrals Subside
Hartikka
I was told by Resperonics folks that Centrals may take up to three months to diminish as a result of CPAP.
RE: How Long Before Centrals Subside
Hi Hartikka. A belated welcome to the Apnea Board from me as well. I am replying to this particular post because of your report of having an AHI of 48 with 10 Centrals. What was the nature of the other AHI events. It is entirely possible that those events were NOT obstructive in nature but were central in nature. When this is the case a CPAP machine converts the central hypopneas to central apneas. These central apneas might show up as Cheyne Stokes Respiration as well as typical central apneas. There very well might be some obstructive events as well especially when on your back. Install Sleepyhead and post some screenshots of your results. This will give us a better idea as to what is going on. As others have suggested you are likely to be a candidate for an ASV machine.
Rich
(01-18-2017, 10:56 AM)hartikka Wrote: Hi SR,
My sleep study was 48 total, or 48 AHI including 10 centrals. With CPAP I went to very little OSA, like .1/hr but still with 10 centrals. So the doctor diagnosed me with severe obstructive. The actual report was 104 hypopneas/hr and 10 centrals for a score of 48 AHI.
The night before last my centrals were 12/hr and 18/hr the night before that. Last night I tried your suggestion of 7 with the EPR off. I only had 2.5 centrals/hr and 2.4 hypopneas/hr. I feel much better so far this morning. The hypopneas went up as i suspected they might, but the trade off seems worth it for sure.
I videotaped my night as well last night and noted that I had 3 times where I started up with a few centrals (they were also less in length at about 13sec each). Each time the centrals started I had moved to the supine. Each time I moved to my side the centrals stopped. Hmm?
The sleep lab had said centrals tend to back off after a couple of months, but the way I've felt the last week was absolutely terrible - worse than no CPAP. It's only one night, but last night was great. Thanks!
I'll keep my eye on that ASV unit and also get set up with Sleepyhead. I'm sure we'll need a good week to see if this change is effective. (Although sleep laps titrate over hours at best.)
Have a good one!
T Hartikka
RE: How Long Before Centrals Subside
[attachment=3158][attachment=3158]

Thanks for everyone's response. Here's a follow up note. I had a cardiopulmonary exercise test where arterial blood gas is checked. My VO2max is down as is my anaerobic threshold. The pulmonary doc said that basically my heart is not keeping up with my legs. I had a stress echo 6 months ago, but I've got another scheduled for tomorrow as they suspect moderate heart disease. Bummer. At 65 I'm 6'1" and 212. I don't look like the "typical" sleep apnea candidate, apparently.
I had lowered my pressure down to 7 (from 10) and turned off the EPR, which brought down the AHI and centrals specifically. Basically my centrals and hypopnea's are equal now, which seems better. However, I'm still all over the map. Last night my AHI was 22 and the night before 6. Average has been around 9. After my exercise test my AHI was 1 for one night. Hmm?
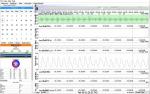
In any event, my centrals and hypopneas are all occuring during very clear Cheyne-Stokes breathing. I've slowly started to increase the pressure, 2 tenths/week. No real trends observed here with that. Pressure is now 7.8. I'm meeting with a sleep tech in a couple of days.
I've attached 2 graphs from last night.
I guess my question is, is the heart disease creating the sleep apnea results? Blood pressure is normal. Ejection fraction was normal 6 months ago. Pulse rate upon waking is 48. Pulse oxygen is 97 upon waking or when tested during the night. I don't have obstructive events. Sleep study said I had 104 hypopneas and 10 centrals per hour. I'm going to need to see those graphs I think. It seems like CPAP is merely trying to correct symptoms rather than treat a perceived primary problem of sleep apnea in my case.
Thanks.
RE: How Long Before Centrals Subside
Cheyne Stokes Respiration (CSR) seems to be a response to Congestive Heart Failure (CHF) that provides rest for the heart. There is only a little when it comes to the reasoning behind this but the thinking is that the heart has to do less work during those periods of breathing cessation. Treating the CSR caused by CHF with ASV machines, especially with an ejection fraction of <45% has detrimental results according to studies. The manufacturers of ASV machines have put out warnings to this effect. My suggestion is that you work with your Cardiologist on treating the CHF. It is possible to treat the Central Apnea with an ASV machine as long as your ejection fraction is >45% (according to the studies) but I am not sure if that is the best thing to due as long as your sleep is reasonably OK and you are not desaturating significantly. I hate to be imprecise about this but there just isn't a lot of literature on the subject. If you are interested you can do a search using Google Scholar on the various topics I have brought up. You will quickly find that most of the research around CSR centers on subjects with CHF.
Rich
RE: How Long Before Centrals Subside
I didn't see this coming, and the Cheyne-Stokes is pretty definitive in your chart. I think you should re-evaluate the LVEF. CPAP is not going to do much to treat these centrals and periodic breathing, and ASV is contraindicated with a LFEF<45%. I don't think there is currently much consensus on ASV in early heart failure where a better ejection fraction is present, but it used to be the gold standard for these issues. We have seen this pattern in some previous members, and unfortunately, this problem exceeds the expertise and ability of members of this forum to help.
Your problems with apnea and periodic breathing are directly related to your heart condition. Any changes, or recommendations should include input from experts that can evaluate your health, and understand how best to treat that. You don't have obstructive sleep apnea, and continued use of CPAP should probably be based on some clinical evaluation of whether there is a benefit (reduction of events) with CPAP compared to just discontinuing use and possibly supplementing oxygen. That last point may be a good question to take back to your doctor. You have a high rate of events, and you should probably have your oxygen desaturation evaluated during sleep to see if supplemental O2 is indicated for when you sleep.
RE: How Long Before Centrals Subside
Hi hartikka,
Let us know the results of retesting your LVEF.
If it was me and my LVEF was still above 45% I would definitely try ASV, because ASV may allow the heart to rest and heal.
Take care,
--- Vaughn
The Advisory Member group provides advice and suggestions to Apnea Board administrators and staff on matters concerning Apnea Board operation and administrative policies. Membership in the Advisory Member group should not be understood as in any way implying medical expertise or qualification for advising Sleep Apnea patients concerning their treatment.
02-06-2017, 09:46 PM
(This post was last modified: 02-06-2017, 09:51 PM by richb.)
RE: How Long Before Centrals Subside
A recent study published in the NEJM points out the potential for negative outcomes when treating CSR in patients with CHF. Granted, the worse the ejection fraction the worse the outcome. http://www.nejm.org/doi/full/10.1056/nej...#t=article
From the Study: "The early and sustained increase in cardiovascular mortality seen in the adaptive servo-ventilation group in this trial was unexpected, and the pathophysiological features of this effect remain to be elucidated. One possible explanation is that central sleep apnea may be a compensatory mechanism in patients with heart failure, as has been suggested previously.19 Potentially beneficial consequences of central sleep apnea, particularly Cheyne–Stokes respiration, in patients with heart failure that could have been attenuated by adaptive servo-ventilation include the resting of respiratory muscles, attenuation of excessive sympathetic nervous system activity, avoidance of hypercapnic acidosis, hyperventilation-related increases in end-expiratory lung volume, and intrinsic positive airway pressure.19 Diminishing this compensatory adaptive respiratory pattern with adaptive servo-ventilation may be detrimental in patients with heart failure, as suggested by the subgroup analysis that showed a positive association between the proportion of Cheyne–Stokes respiration and the adverse effect of adaptive servo-ventilation on cardiovascular mortality.
Another possible explanation is that the application of positive airway pressure may impair cardiac function in at least some patients with heart failure. A number of studies have documented decreased cardiac output and stroke volume during positive airway pressure therapy, particularly when the pulmonary-capillary wedge pressure is low.20-23"
Rich
RE: How Long Before Centrals Subside
I had another stress echo yesterday. The previous one was July 2016. My LVEF is normal - 65, as was the first. The rest of the test was also normal. The doctor said he saw no evidence of heart disease. I had a CPET two weeks ago that saw some evidence of heart disease (reduced VO2 max, etc), thus the stress echo yesterday to confirm. I'm suspecting significant deconditioning and very mild coronary artery disease at the most. My lipid panel is high normal. After a week at a pressure of 7.8 I've had my highest average AHI of over 11. I'm going back to 7, where I've averaged my best AHI, around 6.5. The jury is still out if CPAP is exasperating my therapy by intensifying the apneas to produce centrals. It seems so. My Cheyne-Stokes breathing seems to be averaging about 10%/night. Time in apnea has ranged from 3 minutes/night to 52 min/night. Been on CPAP for about 6 weeks. I can't post screen shots. Apparently the 520k quota is weekly, or something.
I'm seeing a sleep doctor tomorrow where I will go over this data. I'm bringing my laptop with SleepyHead and ResScan results - just in case. It seems to be pointing towards an ASV machine. We'll see what she says. My guess is that it won't be that simple to change to an ASV unit. I'm also starting an exercise regimen - walking up to an hour a day. (This morning it's minus 2F and breezy :-/ so...) I've also ordered a recording pulse oximeter to see where my oxygen goes during this periodic breathing. Everytime I check it when awake, it's 97.
As this progresses, it hopefully will be helpful to others, so I'll keep posting.
Thanks!
RE: How Long Before Centrals Subside
That is great news. You should now focus on the fact you have severe complex apnea syndrome with numerous centrals and periodic breathing resembling Cheyne-Stokes respiration. I would definitely use the data and charts to back this up. You will need an adaptive servo ventilator to resolve this, so give your cardiac health appears relatively good, you need a referral for titration on ASV. Another member recently went through this process and has just had his diagnosis changed from OSA to complex apnea, and is the process of obtaining ASV V http://www.apneaboard.com/forums/Thread-Medicare-Denial . That thread might also be interesting to you.
I'm happy for you and relieved you received some positive news regarding your cardiac health. Hopefully the sleep specialist will recognize the severity of your sleep disturbance with CPAP and order the bilevel ASV titration.
|










