RE: UARS and APAP
(10-24-2019, 02:03 PM)slowriter Wrote: So in comparison, here's PS 5.2, EPAP 6.2.
TV 480, MV 7.13, which appears "normal." Unlike Sleeprider, I think my lungs are pretty normal.
At this point, I'm fine-tuning, but can someone explain what's going on with this wake up event? Is this breathing related that might suggest any settings tweak(s)?
In REM for about 10 minutes (which this shows tail end of), then light, then wake.
The Dreem is telling me I changed position at end of REM, so maybe just that?
..not know much about your sleep stage device. However, your curves, indeed, suggest REM...I don't think would be worth tweaking on this....It would be too minor thing within REM; always with strange bumps in curves..
GL
RE: UARS and APAP
(10-24-2019, 05:57 PM)mper6794 Wrote: (10-24-2019, 02:03 PM)slowriter Wrote: So in comparison, here's PS 5.2, EPAP 6.2.
TV 480, MV 7.13, which appears "normal." Unlike Sleeprider, I think my lungs are pretty normal.
At this point, I'm fine-tuning, but can someone explain what's going on with this wake up event? Is this breathing related that might suggest any settings tweak(s)?
In REM for about 10 minutes (which this shows tail end of), then light, then wake.
The Dreem is telling me I changed position at end of REM, so maybe just that?
..not know much about your sleep stage device. However, your curves, indeed, suggest REM...I don't think would be worth tweaking on this....It would be too minor thing within REM; always with strange bumps in curves..
GL
Yes, you're probably right, now that I look back through other night REM stages. Similar patterns.
So I guess sometimes we more-or-less sleep through that, and other times not, and there's not much to do about it.
RE: UARS and APAP
(10-24-2019, 02:03 PM)slowriter Wrote: So in comparison, here's PS 5.2, EPAP 6.2.
TV 480, MV 7.13, which appears "normal." Unlike Sleeprider, I think my lungs are pretty normal.
At this point, I'm fine-tuning, but can someone explain what's going on with this wake up event? Is this breathing related that might suggest any settings tweak(s)?
I don't have anything to add on the wake up question but the screenshot looks really good.
I noticed your I:E ratio is down to .46 (1.26/2.76) which is pretty low but your TV & MV look great and if your SpO2 was good all night and your getting enough oxygenation I don't see that low I:E ration as a big concern.
How do you feel? / Was it a good night?
INFORMATION ON APNEA BOARD FORUMS OR ON APNEABOARD.COM SHOULD NOT BE CONSIDERED AS MEDICAL ADVICE. ALWAYS SEEK THE ADVICE OF A PHYSICIAN BEFORE SEEKING TREATMENT FOR MEDICAL CONDITIONS, INCLUDING SLEEP APNEA. INFORMATION POSTED ON THE APNEA BOARD WEB SITE AND FORUMS ARE PERSONAL OPINION ONLY AND NOT NECESSARILY A STATEMENT OF FACT.
10-24-2019, 10:53 PM
(This post was last modified: 10-25-2019, 12:10 AM by WillSleep.)
RE: UARS and APAP - Ideas about next steps in for EERS testing.
Continuing the conversation on this post on ideas about next steps in for EERS testing.
http://www.apneaboard.com/forums/Thread-...#pid316403
I continued to do homework trying to find a good reliable ongoing reliable mainstream or sidestream monitoring and data capture solution in existing new or used commercial offerings that was less than $1000. I failed.
However, I did find what looks like a friendly viable path forward.
Five Arduino maker-builder etCO2 monitoring solutions ranging from ~$75-250 USD.
- Sensirion SCD40 (the smallest and most precise, the best sensor to use. Probably far better than most Ventilator CO2 sensors in hospital use today. Announced in May but can not find it for sale anywhere. Cost $200-$250)
- Sensirion SCD30 (Same CMOSense tech used in $1k+ NDIR etCO2 ventilation sensors used by many hospitals today, just at 5-15% of the price they pay. $80 to 120 for an Arduino centric build or $175 for off the shelf plg-in-play kit that connects to PC via USB and comes with graphing software for the PC (15min to setup+time the time to integrate sensor into the hose).
- Grove CO2-Temp-Humid Sensor (built on top of the Sensirion SCD30) (Nice repackaging of the same SCD30 into and ready to use, plug-and-play into the Grove of Arduino ecosystem of products with probably some light scripting work for $80-120. The negative, they increased size of the sensor so might need to trim back the extra PC board to get it right-sized to go into a hose.)
- DFRobot Gravity Analog Infrared CO2 Sensor For Arduino SEN0219 (I am gussing the sensor is not as good but probably good enough and is probably 1-2 hour setup if you follow the "5 min" tutorial they lay out and start by just copying those scripts, all for $80-120).
- Winsen MH-Z19 Infrared OC2 sensor for CO2 Monitor (lowest cost, small sensor, sensor not as good as SCD30 above but probably good enough, scrappy, cheaper than the other options but probably requires the most design and coding work, all for $60-95)
I will post images and a few links on these options on Thursday.
Are there any other good sensor/solution options that we should consider as well or instead?
/////////////////////
Very draft, needs much improvement help from you guys next steps design notes:
Early-draft-needs-your-improvement thinking on SENSOR PLACEMENT ... applies to all etCO2 sensor solution options above:
- Sensor Placement Option 1: Need to be right next to the mask for best effectiveness so add a 2-3 inches of a size hose at the mask or just a few inches down from the mask or extend the existing large section a few inches closer to the mask and locate the sensor inside the section of larger hose that is closest to the mask. I am hoping that with the larger hose the bulk of the sensor will not interrupt airflow (we will need to ensure that it does not) and bulk of the sensor will displace the additional hose capacity that came from adding more large hose.
- Sensor Placement Option 2: The sensors all appear to be directional so can like the bulkier 'mainstream' etCO2 sensors mount the sensors at least primarily outside the hose and look into the hoses through holes or cutouts in the hose. These sensors are not the same shape as off-the-shelf etCO2 sensors so we can not use existing etCO2 off-the-shelf adapters. But it is just hose and so probably not to hard to quickly find a solution that will last just fine for the duration of experiments.
- We may need to ensure the area of the hose the sensors see is mostly free from light.
- The sensors are all expected to be fine with humidity but we may need to sort out how to make sure the sensors do not participate in any 'rain out'. The Stellar 150 accessory guide includes options on how to keep more water out of the line.
Early-draft-needs-your-improvement thinking on WIRES and CONTROLLER PLACEMENT ... applies to all etCO2 sensor solution options above:
- Unlike all the example projects we will expect the sensors will be a good 7 - 9' of wire away from the bus, controller and LCD screen components of our build. The bus, controller and LCD screen components of our build will probably be one unit and rest on the table top near the xPAP machine.
- If the wires were left inside the hose for the 5-6 ' run back to the xPAP they might introduce off-gas, VOC or unwanted noise banging around in side the hose so the wires will exit the hose not far from the sensor and be periodically gently attached to the outside of the hose so they stay out of the way and also are less likely to catch on something. I plan on using a hose cover and you wont even know the wires are there.. may not even know the sensor is there.
Early-draft-needs-your-improvement thinking on DATA, MONITORING and ANALYSIS .. applies to all etCO2 sensor solution options above:
- Will use an LCD panel at the controller so it is easy to validate the sensor is working, to see the current reading and because it it looks really cool, is inexpensive to buy and easy to set up. Lol.
- We will leverage the OpenSource Alarms code that from one of the examples. Careful overnight monitoring and alerting if etCO2 moves out of a safe range is a MUST for testing while sleeping, and the speakers are cheap.
- We will capture and store the ongoing event data in a log file. Any file format and structure Excel can read and Excel can be used for analysis is fine to start.
- Where and how to store the event data as it is occurring is still an open question. Everyone Please reply with suggestions.
- Optional, later if there ends up being long-term ongoing use: We will identify an existing OSCAR file load format to try and leverage as much as possible to make it easier to load the data into OSCAR.
Everyone please reply and help improve those straw dog design notes above.

WillSleep
INFORMATION ON APNEA BOARD FORUMS OR ON APNEABOARD.COM SHOULD NOT BE CONSIDERED AS MEDICAL ADVICE. ALWAYS SEEK THE ADVICE OF A PHYSICIAN BEFORE SEEKING TREATMENT FOR MEDICAL CONDITIONS, INCLUDING SLEEP APNEA. INFORMATION POSTED ON THE APNEA BOARD WEB SITE AND FORUMS ARE PERSONAL OPINION ONLY AND NOT NECESSARILY A STATEMENT OF FACT.
10-25-2019, 05:28 AM
(This post was last modified: 10-25-2019, 05:55 AM by slowriter.)
RE: UARS and APAP
(10-24-2019, 09:15 PM)WillSleep Wrote: (10-24-2019, 02:03 PM)slowriter Wrote: So in comparison, here's PS 5.2, EPAP 6.2.
TV 480, MV 7.13, which appears "normal." Unlike Sleeprider, I think my lungs are pretty normal.
At this point, I'm fine-tuning, but can someone explain what's going on with this wake up event? Is this breathing related that might suggest any settings tweak(s)?
I don't have anything to add on the wake up question but the screenshot looks really good.
I noticed your I:E ratio is down to .46 (1.26/2.76) which is pretty low but your TV & MV look great and if your SpO2 was good all night and your getting enough oxygenation I don't see that low I:E ration as a big concern.
How do you feel? / Was it a good night?
A good night is 8 hours, 1-2 brief arousals.
This was 6:51, with 4 arousals.
So not great.
What settings on the VAuto would impact I:E?
Beyond pressure, I currently have:
Ti min = 0.8
Ti max = 3.0
Trigger = very high
Cycle = high
Edit: looking back through my data, median exp time seems pretty consistent, but insp varies from about 1 to 1.35.
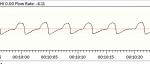
Wiki says sometimes these numbers are miscalculated/reported, so attaching closeup from same night.
10-25-2019, 01:32 PM
(This post was last modified: 10-25-2019, 02:37 PM by WillSleep.)
RE: UARS and APAP
(10-25-2019, 05:28 AM)slowriter Wrote: (10-24-2019, 09:15 PM)WillSleep Wrote: (10-24-2019, 02:03 PM)slowriter Wrote: So in comparison, here's PS 5.2, EPAP 6.2.
TV 480, MV 7.13, which appears "normal." Unlike Sleeprider, I think my lungs are pretty normal.
At this point, I'm fine-tuning, but can someone explain what's going on with this wake up event? Is this breathing related that might suggest any settings tweak(s)?
I don't have anything to add on the wake up question but the screenshot looks really good.
I noticed your I:E ratio is down to .46 (1.26/2.76) which is pretty low but your TV & MV look great and if your SpO2 was good all night and your getting enough oxygenation I don't see that low I:E ration as a big concern.
How do you feel? / Was it a good night?
A good night is 8 hours, 1-2 brief arousals.
This was 6:51, with 4 arousals.
So not great.
What settings on the VAuto would impact I:E?
Beyond pressure, I currently have:
Ti min = 0.8
Ti max = 3.0
Trigger = very high
Cycle = high
Edit: looking back through my data, median exp time seems pretty consistent, but insp varies from about 1 to 1.35.
Wiki says sometimes these numbers are miscalculated/reported, so attaching closeup from same night.
Re: Wiki and OSCAR accuracy of I:E reporting
To me the waveform you posted supports I:E numbers reported I personally would be accepting them as correct. Obviously the OSCAR developers and testers here will have a much more accurate answer to this question than I.
The waveform you posted look:
- Nice and smooth breath-by-breath interaction. No indication in that pic that of Patient<>xPAP algo breath by breath dis-synchronicities. Nowhere are you fighting each other, no missed signals, the jagged edges have a low rate of variability, etc.
- The length of time in Insp and Exh match the means OSCAR reported
- Distance on both sides of Zero is pretty equal
- We can see a bit long expiratory hold at 9:58 and 10:19
- A shorter cycle might help if the CAs you sometimes see happen while your waveforms look like this .... is looks like you are for sure getting enough time to wash out CO2. If all current CAs tie to this waveform then shorting this cycle might be another way to close that those.
The key questions for me are all around if your are getting enough O2 all night.
Not really asking you to answer here..
- How was your O2 all night? Mean SpO2 95%+, low Sat % above 92%, no long periods below 95%, reasonable for you low variablitiy through the night? HR, HRV and curve of HR (looking for a nice hammock curve) through the night good?
- How were TV and MV? Good all night, no ongoing low sections through the night?
If Sp02 was low:
- The last stats you showed indicated you still had ~10% upside to a safe TV max so if you want more oxygenation you might drive for a little more range via EPAP/PS, TiControls, Rise and Cycle.
You have already dialed EPAP and PS into a pretty good balance so I personally would not jump first to make any big changes there (others may have another view).
Update on EPAP/PS settings: All other implications aside higher pressures reduce the breadth of our range and lower pressures help to increase the range of our breath flows. If you were able to preserve all the goodness of the current EPAP/PS balance and get the same or better results averaging 2cm H2O less through the night you would most likely automatically get a little boost in airflow range.
Note that any changes mentioned below may disrupt the current EPAP & PS balance and EPAP and PS might need tuning to return to balance.
High Trigger setting should improve Oxygenation and I would expect tend to not shorten your Insp cycle so I would not change that dial first (others may have another view).
Of the settings below .. either Cycle and Ti Min are the settings I personally would try first.
If you have not recently validated the High Cycle setting I might explore Cycle at Medium and then maybe other settings just to see what it does (or not) to the balance of I vs E, a decrease in CAs and a wee% increase in TV and MV over the last daily results screenshot posted.

If you have not yet done so might try first increasing Ti Min wee bits at a time to see if those changes nicely (or not) create a better balance of I:E, a decrease in CAs and a wee% increase in TV and MV over the last daily results screenshot posted.

Your current Insp waveform shape looks really good so I personally would not jump to Rise first but.. If you have not yet done so might try speeding (lowering the setting) a wee bit at a time to see if it nicely (or does not) creates a better balance of I:E ...

I see that waveform sometimes. Love to hear what you eventually learn best helps.
Update: I just saw this
" Edit: looking back through my data, median exp time seems pretty consistent, but insp varies from about 1 to 1.35."
Were you able to quantify beyond just Insp what else changed, and change in I:E ratio at each time Insp was low might help clear out some noise. Like if both I and E dropped at the same time to 90% of the same degree at that moment then then that event is less significant than when the change between I and E is more divergent.
WillSleep
INFORMATION ON APNEA BOARD FORUMS OR ON APNEABOARD.COM SHOULD NOT BE CONSIDERED AS MEDICAL ADVICE. ALWAYS SEEK THE ADVICE OF A PHYSICIAN BEFORE SEEKING TREATMENT FOR MEDICAL CONDITIONS, INCLUDING SLEEP APNEA. INFORMATION POSTED ON THE APNEA BOARD WEB SITE AND FORUMS ARE PERSONAL OPINION ONLY AND NOT NECESSARILY A STATEMENT OF FACT.
RE: UARS and APAP
Ok.
When I checked quickly earlier, the variation in the insp time didn't obviously correlate to the pressure settings.
Note: rise time isn't available for setting in VAuto mode.
RE: UARS and APAP
(10-25-2019, 04:02 PM)slowriter Wrote: Note: rise time isn't available for setting in VAuto mode.
Thanks! Your rise time looked fine in the waveform above so don't you are missing out.
Cycle set to "High" is literally asking the VAuto to bias to cut short your Inspiration early so setting that back to Medium or less likely even lower might quickly be the trick that settles I:E ratio, maybe some help with CAs, Maybe ups TV a mite..
That is where I would start.
WillSleep
INFORMATION ON APNEA BOARD FORUMS OR ON APNEABOARD.COM SHOULD NOT BE CONSIDERED AS MEDICAL ADVICE. ALWAYS SEEK THE ADVICE OF A PHYSICIAN BEFORE SEEKING TREATMENT FOR MEDICAL CONDITIONS, INCLUDING SLEEP APNEA. INFORMATION POSTED ON THE APNEA BOARD WEB SITE AND FORUMS ARE PERSONAL OPINION ONLY AND NOT NECESSARILY A STATEMENT OF FACT.
RE: UARS and APAP
(10-25-2019, 07:32 PM)WillSleep Wrote: Cycle set to "High" is literally asking the VAuto to bias to cut short your Inspiration early so setting that back to Medium or less likely even lower might quickly be the trick that settles I:E ratio, maybe some help with CAs, Maybe ups TV a mite..
That is where I would start.
Ah, because ideally I want an I:E ratio of 0.5, and so extending the insp time a tad would yield that result?
RE: UARS and APAP
(10-25-2019, 07:53 PM)slowriter Wrote: (10-25-2019, 07:32 PM)WillSleep Wrote: Cycle set to "High" is literally asking the VAuto to bias to cut short your Inspiration early so setting that back to Medium or less likely even lower might quickly be the trick that settles I:E ratio, maybe some help with CAs, Maybe ups TV a mite..
That is where I would start.
Ah, because ideally I want an I:E ratio of 0.5, and so extending the insp time a tad would yield that result?
Changing cycle from high to medium resulted in 1.32/2.44; so 0.54.
TV actually declined slightly, to 460.
This is one night though.

|









