Jadazu treatment thread
Hello everyone,
My history: I have had some kind of sleep disordered breathing for (probably) more than 20 years. (My wife complained about my disruptive snoring back then.) I was diagnosed with obstructive sleep apnea a little less than 20 years ago. The initial diagnosis followed an at home sleep study and two laboratory PSG studies. The laboratory studies were conducted by a sleep disorder clinic. The specialist physician at the clinic prescribed for me a CPAP machine set to 6cm pressure. He acknowledged that the 6cm setting was a guess, as the titration studies did not show any conclusive results. (Unfortunately, I did not know enough to ask for a copy of the studies, and that clinic is out of business now.) I used that therapy for 6 years, renewing the prescription with the same physician each year, and my wife was satisfied that i wasn't snoring.
I did not notice any difference with the CPAP treatment. I was hypertensive and woke up frequently at night. After 6 years of treatment, I bought a Contec CMS50 pulse oximeter and started logging nightly data fron that. I immediately noticed periods during my sleeping, usually 15 to 45 minutes long, of very unstable oxygen saturation levels. The variations were very periodic, about 45 seconds periods, and very regular, cycling from low 90's to low 80's O2 saturation. And when the amplitude of the pattern was smaller, the frequency was about the same; when my O2 saturation was 'stable', in the low 90's, there was usually a 5% fluctuation in saturation with the about the same frequency.
When I showed the sleep doctor the strip charts of these occurrences, about these regular fluctuations, he did not take much interest in them. After i persisted asking about the 'problem', he ordered another PSG study. After the study, (I don't have a copy) the physician prescribed a APAP (Dreamsation) machine, and said that they (he and the respiratory therapist) would use the data fron the machine to define the CPAP therapy. I continued that therapy for another 6 or 7 years. the treatment didn't really improve (and I had another PSG study during that time). The higher pressures with the automatic machine caused me continuous, but inconsistent, problems with air leaking out of my mouth.
Then that sleep clinic went out of business. I next went to a pulmanologist, who is not a sleep disorder specialist, but is the only physician supervising xPAP treatment in my area. He ordered another PSG (I've asked for a copy of that report), and he prescribed another APAP machine, a ResMed S9, with the same suggestion that the data from the machine would be used to evaluate my treatment. This doctor was rather dismissive of my sleeping oximetery data, and called it a "...home science experiment." The new machine had a higher max pressure setting (16cm) and I had severe problems with mouth leakage, the leakage was continous, more or less. I struggled with masks and switched to full face masks.
About two months ago, after five years of struggling with masks and leaks, and looking for ideas and advise, i found this forum. I realized immediately that I had no real idea of how effective my therapy was, and I also realized that I would have to do much more myself to direct my therapy. I downloaded OSCAR and learned, very unpleasantly, that neither of my APAP machines recorded any therapeutic data, that they are bricks. After that denouement, and all that it meant, I went to one of the online suppliers on the list, and bought a ResMed AirSense 10 AutoSet and a ResMed Mini. Ive been recording the machine data for about a month.
Also, I have gone out of the area and 'hired' a new physician, who is a sleep disordered breathing specialist. I was able to show him about one week's Oscar data display, and he knew exactly what it was, and he has taken a very concerned interest in it. He has ordered another PSG, which should happen in about two weeks.
I have recorded about three weeks of nightly data with the A10 (I've used the Mini otherwise). The treatment reports are very inconsistent, without any other factors that I can correlate with the quality of the nightly treatments.
I will attach a couple of examples of daily reports, one of the best and one of the worst. Any advise will be appreciated. Also, any suggestions of questions i should ask or things that I should do in anticipation of the PSG I will be do soon.
Best

Worst
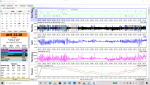

Thank you,
Jim
06-01-2021, 12:57 PM
(This post was last modified: 06-01-2021, 01:15 PM by Jadazu.)
RE: Jadazu treatment thread
Detail from the 'Worst'.

One more of the worst reports:


06-01-2021, 01:09 PM
(This post was last modified: 06-01-2021, 01:10 PM by Geer1.)
RE: Jadazu treatment thread
You appear to have positional apnea. Most commonly caused by chin tucking creating a kinked airway. Pressure is often not capable of resolving this issue and your sleep studies and results have likely been inconsistent because this is only an issue when it is presently an issue.
Read up the following information and consider trying different pillow arrangements, cervical collar and side sleeping (prop yourself up if necessary) to see if that improves the issue.
http://www.apneaboard.com/wiki/index.php...onal_Apnea
Even your best night of data supports the use of a higher min pressure which will help hold airway open a bit more and help minimize the occurrences of these apnea. I would start slow by increasing min pressure to 8 cm for now and focus on trying to treat positional aspects.
RE: Jadazu treatment thread
Thank you.
The 'Worst' night above is with a soft cervical collar. I didn't wake up at all, or I don't remember waking up. I can't say what was happening. I did have the collar on when I woke up, the collar fitting about the same as when I fell asleep.
I am trying different pillows, but I haven't had any consistent results.
I have always been a side sleeper, but usually I wake up when I switch sides. I don't remember waking up the night of that report.
RE: Jadazu treatment thread
The collar may not be high enough or snug enough to stop you from tucking your chin. That definitely looks positional to me, too (though I'm far from an expert). I'm sorry you've had such idiots in the past. It makes me so furious how many doctors are like this.
RE: Jadazu treatment thread
Have you ever tried a nasal mask? If positional treatments don't seem to improve/solve this then that is one of the other things I would try. My grandfather gets unstoppable positional looking apnea with a FFM but doesn't have the issue when using nasal masks (just leaks like a sieve through his mouth...).
06-02-2021, 12:37 PM
(This post was last modified: 06-02-2021, 12:50 PM by Jadazu.)
RE: Jadazu treatment thread
Ratchick, I'm not yet confidant that the collar is adequate. The foam is compliant. I'm still struggling with the discomfort of wearing it.
Geer1, re the nasal mask, your question makes me remember something; the first doctor I went to said that he thought FF masks were problematic as the mask pulls the jaw rearward. One of the treatments that that doctor also prescribed were jaw advancement devices.
I do still have nasal masks and cannulas. When I used the nasal masks, my mouth leaks were almost unstoppable. I slept with a pillow stuffed under my chin, which reduced the leaks (and probably improved my head position) but keeping the pillow under my chin was difficult. WRTT, how much mouth leakage is too much?
Strangely, when I was using the nasal mask I was not sleeping as well as I do now as I woke up frequently to roll from side to side, but I did not feel tired during the day. Now, using the FF mask, I sleep through the night usually, but I'm very tired during the day. (There may be no other cause of this than that I am about five years older...) Trying to resolve the sleep quality and sleep state question, I've been thinking about getting a fitbit-like wristwatch sleep quality monitor. Does anyone have an opinion of their utility and accuracy?
Another question I have is a speculative one about my sleep breathing. Much of the time that I am breathing 'well', I can see a slight rhythmic pattern in my breathing. The tidal volume and SpO2 show the rhythmic variations.

When I have clusters of apneas, a similar rhythmic pattern seems to be happening.

The speculative question that i have is if the clusters are happening as an airway restriction, not necessarily an obturation, is continuously happening. That is, if an increased impedance is pushing the lower volume parts of my breathing pattern below a threshold? Is the positional problem a continuous airway restriction? (OSA has been explained to me as being periodic momentary obstructions of the airway.)
Thank you,
Jim
ETA: These thing weren't flagged, but they seem like impeded breathing.

RE: Jadazu treatment thread
The rhythmic breathing you mentioned is what I would call periodic breathing and it is commonly central in nature but it can also be obstructive. In your case there is enough support to believe obstruction is a primary concern so I would focus on it first then if the periodic breathing or central apneas continue then can look into treating them.
The cluster of apneas you posted are definitely obstructive in nature even though there are some improperly flagged "central" apneas.
The last example you posted are RERA's, you have worsening flow limited breaths that ultimately end up in arousal (large recovery breaths are after the arousal). Since there is no cessation of flow they aren't obstructive apnea and because the reducing of flow occurs slowly they aren't even being flagged as hypopneas.
I have a couple theories on FFM's and pushing jaw back is one of them, the other is pressure inside mouth pushes back and down on tongue etc. Mouth leaks are an issue but there are different ways to try and deal with them. As a test to see if you do better on a nasal mask I would switch to one of your nasal masks and in order to avoid mouth breathing/leaks you can tape your mouth closed (using medical style tape). Fold a little flap on one end so you can easily remove the tape if you need to.
RE: Jadazu treatment thread
Geer1,
Thank you.
I will use the nasal mask again, and look at the reports for a few nights. And I have another soft collar to try.
thank you,
Jim
06-17-2021, 09:37 AM
(This post was last modified: 06-17-2021, 09:39 AM by Jadazu.
Edit Reason: ETA
)
RE: Jadazu treatment thread
Hello everyone,
In the progress of my treatment, I had my recently scheduled PSG study on Monday night. The sleep lab is owned by / part of the big regional hospital's health care providing system. To do the sleep test, I went to a multi million dollar facility, to have a several thousand dollar test done on me, and they made me sleep on a $50 mattress. The bed in the lab sleep room was a fold-up Murphy bed, a glorified futon, one of those cheap imported things sold on ebay, with a thin and hard batting mattress, i.e. a pallet. With cheap pillows. Truly awful and uncomfortable. It's just amazing, to me, that the people responsible for operating the sleep laboratory think that a fold-away bed is adequate for the subject of a *sleep test*, to sleep on... A budget priced motel couldn't getaway with providing a bed like that.
I'm a side-sleeper, so I slept about three hours before the shoulder and back and hip pain keep me awake the rest of the night. With no advil available, as I didn't think to bring any...
I have a success to report, that happened prior to the incident recounted above. At the suggestion of the members here (Thank you!), I've been wearing a soft foam cervical collar while sleeping. And doing that has been made very large improvement in my treatment. It has reduced the flow limitations considerably and, I think, reduced the restricted or impeded breathing I was having.
Last nights report is fairly typical of the recent ones, when I've been wearing the soft cervical collar. I am using an EPR setting of 3. The AHI's have been in the 5-8 range, which is a third or quarter of what they have been previously.
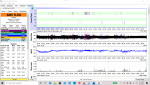
Periodic breathing is something I am still having.


I am interested in any interpretations of this, and any suggestions about this.
Thank you,
Jim
ETA: I have been using a nasal cannula mask.
|









